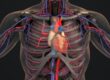
The MIS TLIF (Minimally Invasive Transforaminal Lumbar Interbody Fusion) procedure takes a gentle approach to the spine, utilizing a small incision in the patient’s back, typically only about an inch long. Unlike traditional methods, this technique navigates between muscles instead of stripping them from the bone, significantly reducing surgical muscle dissection and nerve movement needed to access the vertebrae, discs, and nerves. This results in a less traumatic experience for the spine, safer conditions for nerves, and opens the door for minimal access and endoscopic techniques for spinal fusion. The decreased trauma to soft tissues often leads to benefits such as decreased blood loss, shorter hospital stays, and a quicker recovery.
The MIS TLIF (Minimally Invasive Transforaminal Lumbar Interbody Fusion) procedure takes a gentle approach to the spine, utilizing a small incision in the patient’s back, typically only about an inch long. Unlike traditional methods, this technique navigates between muscles instead of stripping them from the bone, significantly reducing surgical muscle dissection and nerve movement needed to access the vertebrae, discs, and nerves. This results in a less traumatic experience for the spine, safer conditions for nerves, and opens the door for minimal access and endoscopic techniques for spinal fusion. The decreased trauma to soft tissues often leads to benefits such as decreased blood loss, shorter hospital stays, and a quicker recovery.
When is Lumbar Spine Fusion Recommended?
Lumbar spine fusion may be suggested for individuals with debilitating low back and leg symptoms that have not improved with non-surgical treatments. Conditions like spondylolisthesis, degenerative disc disease, or recurrent disc herniations often cause mechanical pain, making them potential candidates for spinal fusion. The TLIF procedure is designed to address the disc as a source of mechanical back pain.
Preparing for Surgery: What to Know
Before the surgery, thorough preparation is crucial. A complete physical exam ensures good health, and tests such as blood work, EKGs, and chest X-rays are conducted. Discuss all medications, including prescription, over-the-counter, and herbal supplements, with your healthcare provider. Medications that thin the blood should be stopped, and alcohol consumption should cease a week before and two weeks after surgery. Quitting smoking is essential for successful fusion, as nicotine can hinder bone growth.
During the Surgery: What to Expect
Under general anesthesia, the surgeon makes a posterior incision to access the back of the spine. Care is taken to preserve muscle tissue, and any structures like bone spurs are removed to relieve nerve compression. The facet joint is then removed to reach the disc with minimal nerve manipulation. Most of the disc is removed, creating space for bone grafts. A cage, typically made of metal or other materials, is inserted to maintain disc space height. Bone grafts, a combination of patient’s bone and from a bone bank, promote fusion over time. Additional bone is placed laterally to enhance fusion, and the area is immobilized using plates, rods, screws, or cages. After closing the incision, the patient is taken to recovery.
After Surgery: Recovery and Follow-up
Patients are often discharged on the same day as surgery, with rare need for blood transfusions. Physical therapy begins around two weeks after surgery, and patients are gradually mobilized, sometimes with the aid of a spinal brace. Follow-up with the surgeon occurs in several weeks, during which the surgical dressing is usually removed. Patients can start showering the next day but should avoid soaking the wound until fully healed. Return to office work is typically in four to six weeks, depending on the nature of the job. Activity levels increase with physical therapy as the fusion heals, which can take around 6-7 months for functional improvement. Complete fusion may take a year or longer.
Contact Us