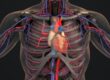
The three types of back pain to be aware of are nerve, muscle, and bone. When you have back pain, it can change everything in your daily life. Your back can tell you a lot about your health and by being able to identify the differences in your pain, you can get back to living your life. Being able to detect and determine your pain can help you live a healthy and in-tuned lifestyle. Continue reading below to learn more.

Pain is defined as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage,” according to the International Association for the Study of Pain. While it’s unpleasant, pain is the body’s way of alerting you to a problem, thanks to specialized peripheral sensory neurons called nociceptors. These neurons detect potential or actual damage and transmit the information to the brain. When the brain processes that information, you feel pain.
Musculoskeletal pain, which is usually what back pain is, comes in a couple of varieties, such as:
- Nerve or neuropathic pain
- Muscle and ligament pain
- Bone and cartilage pain
Being able to tell them apart can help both patients and doctors figure out what to do about them.
“[Pain] is the most common [patient] complaint, but it all needs to be put in context and determine as to what is the cause of the problem,” says a professor of anesthesiology and Vice Chair of Research for the Department of Anesthesiology at Rush Medical College in Chicago, IL, and the immediate past president of the American Association of Regional Anesthesia and Pain Medicine.
Nerve Pain
According to doctors, nerve pain is often described as shooting or radiating pain. Your doctor might call it radicular pain or radiculopathy. That’s because it shoots away from the spine and spinal cord and radiates down the path of a nerve.
“When you have radiating pain, it’s generally from the lumbar spine to the legs, and from the cervical spine to the arms, forearms, and hands,” an expert says. “So you may have disc herniation that can cause pushing on the nerve roots and that’s when people have the pain going down their extremities, to the legs or to the hands.” Sciatica is a common example of radiating pain.
Treating this kind of chronic pain requires relieving the pressure on the nerve root. A surgeon may clear out the herniated part of the disc that’s actually pressing on the nerve in a minimally invasive procedure called a microdiscectomy, if you’ve had this kind of nerve pain for a long time. But, most cases resolve themselves after a few weeks (cold comfort when you’re in the middle of it, we know).
Muscle Strains and Ligament Sprains
Have you ever sprained a ligament or strained a muscle? Maybe you rolled your ankle or pulled something from strenuous activity. Strains are painful injuries or irritation of muscles or the tendons that attach them to bone, while sprains are similar injuries to ligaments, tough tissue that binds bones together.
In the back, you might strain your:
- Latissimus dorsi (lats)
- Trapezius
- Erectors spinae
- Rhomboids
…and many others. There are also two ligaments that run the length of your spine called the anterior longitudinal ligament and posterior longitudinal ligament, plus ligaments that connect each vertebra to the ones above and below it. Generally, the anterior and posterior longitudinal ligaments do not get sprain. Injuries to these ligaments are usually significant and associated with additional spinal injuries.
“Muscle pain is more of an ache, and it’s most often felt with movement—turning around, for example, would typically produce that,” says doctors. Most muscle pain can be helped with simple home care, such as Ace bandages, ice packs, elevation, and RICE:
- Rest
- Ice
- Compression
- Elevation
For many people, it’s the “rest” part that is the hardest and also the most important. It’s a problem, experts recognize. “Most people, in four to six weeks, they’ll get better. But I realize that four to six weeks is a long time for some people. But people do do it.” Ligaments generally heal the same way as muscles, but usually a bit slower.
Fractures and Bone Spurs
Bone pain is the least common of the three types of pain in this article. Fractures (broken bones) cause very obvious bone pain, but there are other medical issues that may also be causing that deep down kind of ache.
“Bone pain is more of a constant ache,” explains an expert. It can often be caused by osteoarthritis, which is called spondylosis when it’s in the spine. In osteoporosis, the cartilage that protects the bones in a joint degenerates, which can cause bones to painfully grind against each other, as well as develop bone spurs that can crowd the spinal canal and cause nerve or radicular pain.
Osteoporosis, a condition that causes bones to weaken and become more brittle, is another common cause of bone pain in the form of fractures. More than 10 million Americans have it, with another 44 million at risk for it. Osteoporosis of the spine puts you at risk for compression fractures, where weak vertebrae collapse.
Other potential causes of bone pain are more serious, including osteomyelitis (infection in a bone) and certain types of cancer, including leukemia. But most of the time, it’s something far less frightening, assures an expert.
“Generally, if you look at 100 people, it’s more commonly degeneration or arthritis that causes bone pain,” a doctor says. You should be concerned about it, but again you should be looking at common things before going to think of the rarer stuff.”
What to Do About Back Pain
Deciding when to see your healthcare provider about pain depends on many things, but for some experts, it’s really a question of quality of life. “Yes, everybody has aches and pains here and there,” one says, “But what is it preventing you from doing on a day-to-day basis? I think that provides a good measure of quality of life.”
If back pain is preventing you from normal activities such as getting dressed, driving, reaching for or picking up things around the house, or similar everyday motions, it’s time to call a doctor. The right diagnosis of what kind of pain you are having is the first step to getting the right treatment. That treatment may include medication (anticonvulsants or muscle relaxers, for example), interventional devices such as spinal cord stimulators, physical therapy, or even surgery.
Your primary doctor may also recommend seeing a pain management specialist. “A pain management physician is someone who understands the pathophysiology of the disease or the condition [causing the pain.” This type of specialist is also more aware of both medications and interventional options that can have a positive effect on pain.
Pain may be a fact of life, but back pain doesn’t have to stop you from living your life. Now that you know about some different types of back pain, you’re better equipped to take an active role and be a partner in your own healthcare.
Original and complete article published on spineuniverse.com