 What is degenerative disc disease (DDD)? The discs in the spine are the soft cushions that allow our back to move. They are shock absorbers that give the bones (vertebrae) above and below the ability to mobilize. DDD occurs throughout life and is comparable to the normal wearing process known as arthritis. The forces that drive the aging process are; loss of cells, loss of water content, loss of proteoglycan content, decreased collagen, increased fissures in the disc known as annular fissures, mechanical incompetence, and bony changes. These changes are known as the Thompson criteria. In summary, all of the substances that give the discs its ability to function as a shock absorber begin to decrease overtime.
What is degenerative disc disease (DDD)? The discs in the spine are the soft cushions that allow our back to move. They are shock absorbers that give the bones (vertebrae) above and below the ability to mobilize. DDD occurs throughout life and is comparable to the normal wearing process known as arthritis. The forces that drive the aging process are; loss of cells, loss of water content, loss of proteoglycan content, decreased collagen, increased fissures in the disc known as annular fissures, mechanical incompetence, and bony changes. These changes are known as the Thompson criteria. In summary, all of the substances that give the discs its ability to function as a shock absorber begin to decrease overtime.
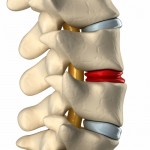
DDD is seen on imaging (MRI, CTs, X-rays) but it not clinically important until a person becomes symptomatic from the findings. It is quite impossible to fix normal, so if findings do show up on imaging, they do not need to be treated until a person is truly in pain from those findings. The MRI is the most sensitive modality to diagnosing and staging degenerative disc disease. The stages are based off the progression of the degeneration. disc height and loss of water/proteoglycan/collagen content provide changes that can be seen on an MRI. For instance, disc height is looked at throughout the spine to compare normal discs with discs that may be degenerative. Also the content of the discs provide changes in color of the disc indicating a loss of the internal components that give the disc its spongy structure. These changes help place a patient into a stage of degeneration to mark how significant the condition is and gives the provider ability track its progress.
 The symptoms usually experienced with degenerative disc disease are; neck pain, back pain, and buttock pain. If leg or arm pain is present, there is likely an additional cause such as a herniated disc or stenosis. These additional symptoms would indicate that DDD is not the sole diagnosis.
The symptoms usually experienced with degenerative disc disease are; neck pain, back pain, and buttock pain. If leg or arm pain is present, there is likely an additional cause such as a herniated disc or stenosis. These additional symptoms would indicate that DDD is not the sole diagnosis.
Treatment is initially focused on conservative measures such as rest for acute pain, NSAID medications, and physical therapy. Surgical treatment is considered after failure of non-operative treatment usually at minimum of six weeks. Surgical options include fusion procedures and disc procedures. A fusion operation includes removing the disc and fusing two bones (vertebrae) into one. Disc replacement includes removing the disc and replacing it with a device that allows the specific area to maintain motion instead of fusing the vertebrae solid. Each procedure has its pros and cons. If surgery can be avoided, it should. Conservative measures are always preferable; however some patients do eventually need a procedure to fix their condition. At Prairie Spine and Pain Institute we offer every option for our patients, and place them in control of their care, and not the other way around. Degenerative disc disease is one condition that we are dedicated to treating at Prairie Spine and Pain Institute.
About The Author: Derek N. Morrow, PA-C is a physician assistant with Prairie Spine and Pain Institute. Derek works in the clinic setting as a health care provider seeing patients. He is also utilized in the operating room as a first assist in surgery. In the clinic setting, his key function is to diagnose new patients and conduct their initial treatment. He works directly with patients to establish customized treatment programs and to monitor their progress. He also conducts history and physical evaluations for many patients. He performs many office procedures including trigger point injections, large joint injections, and bursa injections, all with the help of ultrasound guidance. He is radiologically trained, and uses his knowledge of X-ray, Ultrasound, MRI, CT, and EMG-Nerve Conduction Studies to establish a diagnosis and determine the appropriate treatment. Derek is surgically trained and plays a vital role in the procedures we perform at Prairie Spine and Pain Institute.