We humans are fragile creatures, and no part of our anatomy bespeaks our frailty quite like the lower back.
The neighborhood where spine and pelvis meet is a marvelously complex arrangement of bone, nerve, muscle and connective tissue that holds us upright, yet provides a remarkable range of motion and flexibility. So it’s no wonder that things go wrong sometimes when we bend over to tie our shoes or pick up a bag of trash. Lucky and rare are those folks who haven’t felt the jolt of searing pain that announces an episode of low-back pain.
The natural response when your back “goes out” is to lie down and wait for the pain to go away. It turns out that course is exactly the wrong one for most of us. New guidelines for treating low-back pain encourage people to stay active to promote healing, avoid expensive imaging tests and use ordinary over-the-counter medicines to control pain while they’re on the mend.
Back pain is one of the most common complaints physicians treat — right up there with sore throats, says Dr. Paul Matz, a family practice physician at Medford Medical Clinic. Unfortunately, Matz says, there’s not a whole lot of evidence that aggressive medical treatments hasten healing for most people.
“Ninety percent of people get better with time,” he says, but studies show little difference in recovery rates among those who seek chiropractic care or physical therapy compared with those who do nothing special.
The new guidelines were developed by a partnership led by Oregon Health Care Quality Corporation (often shortened to Q Corp), a nonprofit organization that seeks to improve health care by producing unbiased information. The guidelines were developed “to help people get the right care when they need it,” says Mylia Christensen, Q Corp’s executive director.
The goal is to help people manage low-back pain without having to undergo tests and treatments that may not benefit them and that have the potential to do harm, Christensen says. Q Corp will produce additional treatment guidelines as part of the health reform plan created by the Oregon Health Policy Board under the provisions of the Legislature’s 2009 health care reform law.
The new low-back guidelines are available on the Web here.
“The pamphlet is very well written,” Matz says. “I wish more people would follow its advice.”
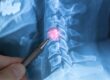
He supports its statements that most people suffering from ordinary low-back pain don’t need expensive imaging tests such as MRI or CT. That’s because the pictures generally don’t provide information that explains the pain.
“The level of detail you can see is amazing,” he says, but there’s a very low correlation between what the pictures show and how the patient feels. “The connection between the pictures and why the patient hurts is 15 out of 100.”
He tells a story to illustrate the point. When MRI was a relatively new technology, some patients’ back images showed structural abnormalities such as bulging spinal discs, and physicians assumed those irregularities were associated with the pain. Later, as more images were made of people without back pain, physicians learned a large majority of normal healthy people also have bulging discs or other spinal abnormalities.
The guidelines also encourage people with low-back pain to keep moving to promote recovery. Severe pain may dictate a day or two of rest, but activities such as gentle walking, swimming or pedaling a stationary bike encourage healing by increasing blood flow through the injured area, says Bruce Mendelson, a physical therapist at Providence Medical Plaza Central Point.
“If you don’t do much, circulation around the pain (area) ceases,” Mendelson says. “You need to get the circulation going.”
Regular physical exercise also has been shown to help prevent low-back pain, Matz says. “Two things are very beneficial — walking on a regular basis and abdominal strengthening exercises such as crunches.”
He says it’s important to get adequate restorative sleep to promote healing. Over the course of a normal sleep cycle, the body has several episodes of deep sleep when the muscles are essentially paralyzed, “and there’s some evidence that’s where lots of muscle healing comes in.” If pain is interrupting sleep, a physician can prescribe appropriate medicines.
The guidelines recommend people treat their low-back pain with over-the-counter medications such as acetaminophen (Tylenol is one brand name) or any of the class of drugs called non-steroidal anti-inflammatories, such as aspirin, ibuprofen (Advil and others) or naproxen (Aleve and others). Narcotics provide stronger pain relief, but they can be addictive, and their side effects, such as drowsiness, can cause other problems for people who need to think clearly or operate machinery.
Mendeslon describes the guidelines as “basically stuff we say (to patients) every day,” but he says the information can help people with back problems “reset the way they think about back pain.”
Source: www.mailtribune.com; Bill Kettler; March 4, 2012.